Biolight ST is designed to offer the highest quality of design and materials, but with the realization of additional cost savings. Biolight ST uses a material that is not quite as radiopaque as Biolight DUAL, but will still matches or surpasses other brands of high-radiopacity fiber posts. In addition, Biolight ST drills and posts are of a simpler taper design, which is still chosen by many clinicians, but is easier to manufacture.
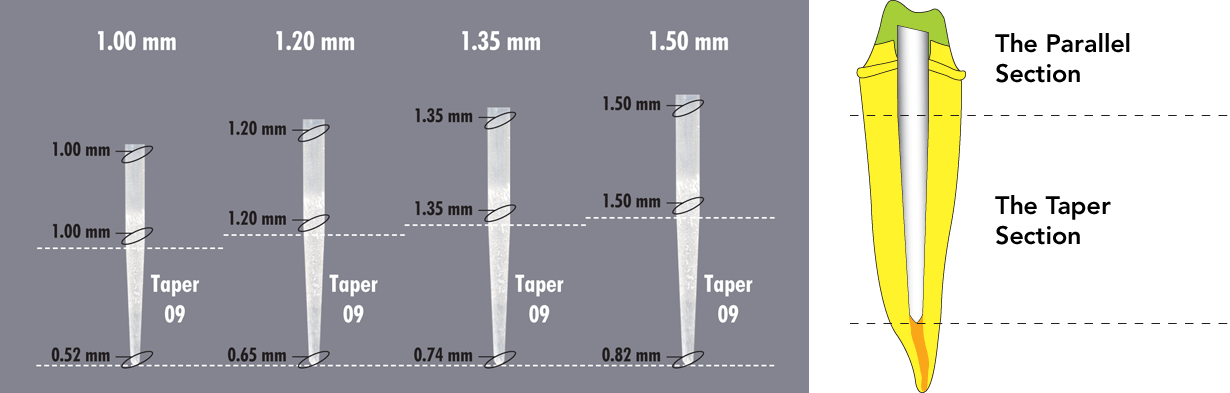
The coronal portion of Biolight ST is parallel, while the apical portion is a taper design. This permits the clinician to choose a larger coronal diameter for increased strength, while the conservative taper portion minimizes the amount of dentin reduction.
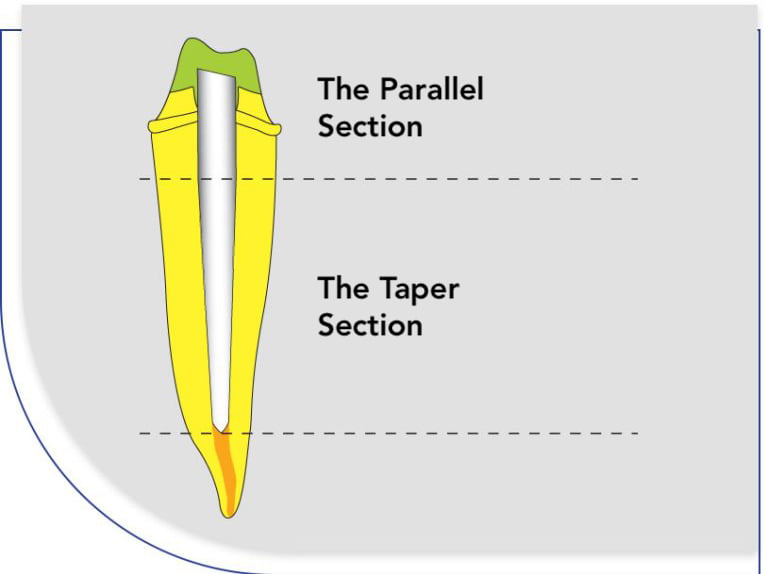




All Biolight products are manufactured without the use of either Epoxy or Bis-GMA resins.
The materials used to make Biolight ST posts excel in independent studies and evaluations. (see below)
A recent independent university study comparing the shear modulus of various fiber posts produced these results:
Force required to BREAK post (MPa)
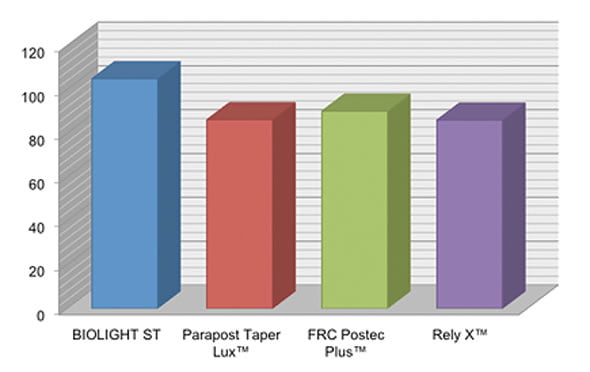
| BIOLIGHT ST: | 104.81 MPa |
| ParaPost® Taper Lux: | 86.12 MPa |
| FRC Postec® Plus: | 90 MPa |
| RelyX™ Fiber Post: | 85.94 MPa |
® or ™: Registered trademarks or trademarks of their respective manufacturer.
In the same independent evaluation, the Biolight material against exhibited superior radiopacity to all competitive fiber posts tested.
Radiopacity of fiber posts
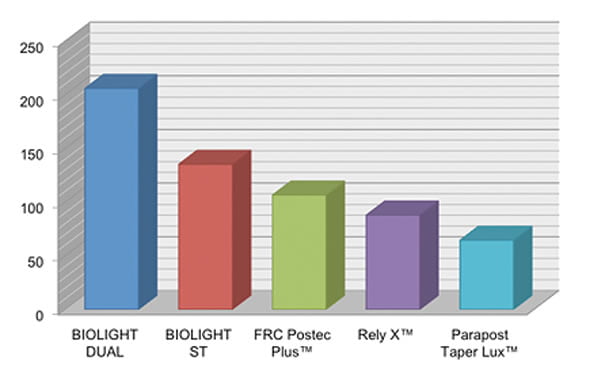
| BIOLIGHT DUAL: | 205.90 |
| BIOLIGHT ST: | 135.42 |
| FRC Postec® Plus: | 106.67 |
| RelyX™ Fiber Post: | 88.04 |
| ParaPost® Taper Lux: | 64.67 |
® or ™: Registered trademarks or trademarks of their respective manufacturer.
There is a long history and continual evolution in the materials and shapes used to manufacture dental intra-radicular posts.Early attempts at prefabricated metal posts contributed to root fractures as they were designed to replicate custom cast posts and were manufactured with a wedge shape. Upon mastication, forces were transmitted through the root, causing a known problem of root fractures. This led to the development of parallel-shaped metal posts which have been in use for decades now. The parallel shape eliminated this wedge effect and was a statistically superior solution. However, obvious limitations persisted. To insert a parallel post into a tapered canal means one of two things (or in many cases – both): Unnecessary reduction of tooth structure in the apical portion of the canal will weaken the root at the tip of the post, and increases risks during post space preparation. If a smaller diameter post is chosen, then the coronal portion of the post must be filled with cement. The cement is the weakest link in the solution and doesn’t offer much support for the crown. Several other metal post designs were then developed to deal with these issues, however others were turning to fiber-resin solutions, which have since dominated post developments. The 1st post design introduced by Synca, Logipost-UM, was evaluated by a well-known American independent research institute in 1998. Even with this early version, 92% of evaluators rated the product as excellent or good. It virtually eliminated the potential of root fracture, as the fiber exhibited the same modulus of elasticity as dentin. It was not parallel, but offered a .02 taper, which was a step in the direction of anatomical design. Lastly, the fiber-resin in the posts bonded to current dental bonding materials, creating the potential to reinforce remaining tooth structure following root canal therapy. These early designs were immediately adopted by many clinicians, but still had limitations. They were radiolucent. When looking at an x-ray, one could think that the clinician had created a post room, but failed to insert the post. They were made from black carbon fiber. This potentially created a problem in esthetic anterior restorations. Lastly, the post shape, though somewhat anatomical, did not fully exploit the properties of fiber to design the most anatomical post possible. Early commercial success of fibers posts led to a multitude of products to flood the market. All are somewhat successful to a varying degree, however, unlike stainless steel, all fiber is not created equally. There are significant differences in both the materials used and the shapes of current fiber posts. Irrespective of posts that are used, current literature maintains that 2mm of remaining tooth structure or ferrule preparation are key factors in clinical success. In addition, the overall minimal reduction of healthy tooth structure has been noted as the most important factor in clinical success. While some literature questions the need for posts when ferrule preparation is present, other literature supports the increase in fracture resistance and an overall strengthening of the tooth when a post is placed. Studies which have compared different post diameters in the coronal area have noted an increase in fracture resistance. Studies that evaluated resistance to breakdown from fatigue could be more pertinent. Regardless of the frequency that the clinician chooses to place posts, it is important to remember that all fiber posts are not created equally. The two most important factors are the shape of the post and the physical properties of the post material. |
Why settle for problems?
|
Fiber Posts are much Closer to Human DentinFiber posts exhibit physical properties that are much closer to human dentin than any metal. As a result, they virtually eliminate the risk of root fracture.
Comparative analysis of modulus of elasticity (GPa)
|
Transmit LightFiber posts transmit light to start the polymerization process. Fiber posts must be placed with either dual-cure or self-cure resin cements. If using a dual-cure resin cement, the curing process is expedited, and holds the post in place while the self-cure process completes itself.
|
Anatomically ShapedFiber posts can be anatomically shaped for maximum clinical success. Since fiber posts do not cause root fractures, they can be designed and shaped to meet ideal anatomical demands – smaller apical portion, wider coronal support, taper design, etc. |
More EstheticFiber posts are esthetic. The material used to make BIOLIGHT posts blend in with the natural tooth colored restorations. |
Possibility of RetreatmentFiber post failures are non catastrophic and are repairable. Generally in the case of post and core failure using fiber posts, the post will either break or de-bond. A metal post failure will often include a root fracture and will require extraction. |
Monobloc RestorationFiber posts provide a monobloc restoration. In other words, the post bonds to the resin cement and the resin cement bonds to dentin. All BIOLIGHT posts are made from UDMA resin and will both chemically and mechanically bond to all resin cements used today. In addition, BIOLIGHT DUAL posts have a unique micro-roughened surface for superior adhesion. |
Why are BIOLIGHT posts made from E-glass in a UDMA resin?Between 2001 and 2007, the 2nd generation Synca posts were made from a Quartz glass in an epoxy resin. At that time, quartz glass/epoxy resin offered superior fracture resistance and resistance to breakdown in cyclical fatigue testing over other manufacturers. In 2004, an independent testing institute showed that a post using E-glass in a UDMA resin exhibited the best fracture resistance overall. In this 2004 study, all esthetic fiber posts are classified together as glass fiber. In addition, an important cyclical fatigue study published in Dental Materials showed that only 2 post manufacturers, namely the 2nd generation and 3rd generation fiber posts sold by Synca, were able to produce posts that resisted over 3,000,000 cycles of fatigue. All other brands (including: ParaPost® Fiber White, FibreKor™, Luscent Anchors™ and Snowpost) failed. Since 2008, Synca posts are now manufactured from the E-glass/UDMA resin matrix. This maintains all the benefits of the 2nd generation product, while offering several advantages. What is the difference between E-glass and Quartz-glass?Both these glasses are used in a variety of applications and have the same main ingredient: SiO2. With respect to dental posts, performance is not related at all to the type of glass used. It is relative to the combination of glass fiber/resin matrix and the processes used in manufacturing. |
What are the other advantages of SYNCA Post?1. Higher radiopacity:
2. Higher bonding with self-adhesive cements:
3. No need to prepare surface for bonding/resin cement: Previous studies with Quartz glass/Epoxy posts showed that surface treatment (H2O2 and Silane) was necessary to achieve highest bond strengths.
4. Biocompatibility: |
(1) Mentlink A.G., Meenwisser R., Kayser A.F., Mulder J. – Survivial rate and failure characteristics of all metal post and core restorations. – J. Oral Rehabilitation, 20. – 1993. – 455-461
(2) Asmussen E., Peutzfeld A., Heitman T. – Stiffness, elastic limit and strength of newer types of endodontic posts. – J. Dent, 27. – 1999. – 275-278
(3) Fatigue resistance of different type of fiber posts. – University of Sienna. – Livorno. – Italy
(4) A shift away from metal. – CRA Newsletter Posts. – May 2004
(5) Pierre Boudrias, DMD, MSD, Salam Sakkal, DMD, MSD, Yuliana Petrova DMD. – Anatomical Post Design Applied to Quartz Fiber/Epoxy technology: A conservative approach. – Oral Health, November 2001. – 9-16
(6) Goodacre C.J., Spolnik K.J. – The Prosthetic management of endodontically treated teeth: a literature review. Part 1 success and failure data, treatment concepts. – J. Prostho, 3. – 1994. – 243-250
(7) Pierre Boudrias, DMD, MSD, Salam Sakkal, DMD, MSD, Yuliana Petrova DMD. – Anatomical Post Design Meets Quartz fiber technology: Rational and case report. – Compendium, April 2001. – 337-348
(8) Shadman S., Sadat Sabei N., Gardus M., et al. – Endo-composipost UM canal adaptation in endondontically treated teeth. Supervised project. – University of Montreal. – 1999.
(9) Dental Materials Volume 21, issue 2, February 2005. – 75-82
(10) CRA NEWSLETTER, May 2004.
(11) RadTech Europe 2005 Conference & Exhibition
(12) Julio Mesquita Filho. – University of Toronto in association with University Est. Paulista. – Sao Paulo, Brazil. – 2007.
(13) Annet Kutesa-Mutebi, Yusuf I Osman. – Effect of the ferrule on fracture resistance of teeth restored with prefabricted posts and composite cores. – Afr Health Sci., August 2004. 4(2): 131-135
(14) Jelena Juloski, DDS*, Ivana Radovic, DDS, MSc, PhD†, Cecilia Goracci, DDS, MSc, PhD*, Zoran R. Vulicevic, DDS, MSc, PhD†, Marco Ferrari, MD, DDS, PhD* – *: Department of Fixed Prosthodontics and Dental Materials of Siena, Tuscan School of Dental Medicine, University of Florence and Siena, Siena, Italy. – †: Clinic for Pediatric and Preventive Dentistry, Faculty of Dentistry, University of Belgrade, Belgrade, Serbia – Ferrule Effect: A Literature Review – Journal of Endodontics – Volume 38, Issue 1, January 2012, Pages 11-19